The latest in a series of headline-making pig-to-human transplants, saw a 56-year-old man with liver failure connected to a genetically modified pig liver outside his body. The pig organ filtered the man’s blood for a few days while he waited for a human liver transplant. The research community is watching closely as these xenotransplants hold the promise to reduce the number of people who die while waiting for a human organ, and ultimately end the world’s organ shortage as a whole. Currently, less than 10% of the global organ transplantation need is met, according to the World Health Organization.
Pig tissues are already routinely implanted in humans across the globe. Every year, some 60,000 patients in the US benefit from pig tissue transplants in the form of heart valves. Scientists started small, first successfully transplanting a few animal cells into humans, before further exploring the potential of whole organ transplants. In 2021, surgeons successfully transplanted for the first time a genetically altered pig kidney into a brain-dead patient with no hope of recovery. Since then, several more pioneering surgeries have been performed. About half a dozen people in the United States and China have received organs from genome-edited pigs — kidneys, hearts, liver and a thymus - on compassionate grounds and several clinical trials are underway to produce crucial safety and efficacy data.
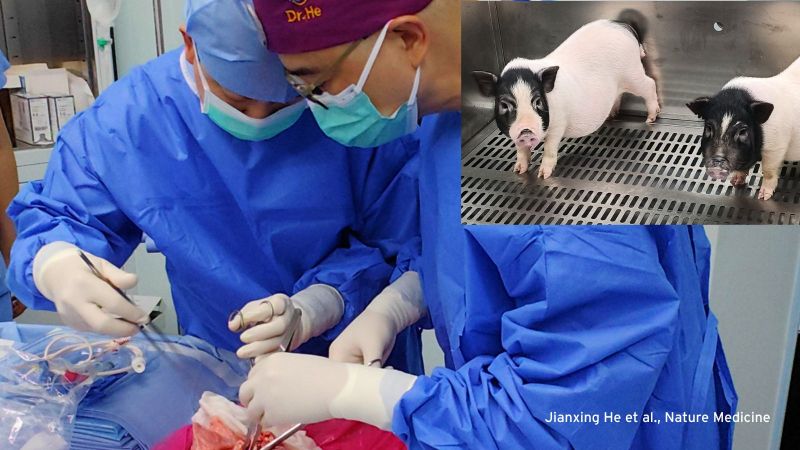
This latest surgery is somewhat original but nevertheless crucial in determining the potential of xenotransplants for human patients. The recipient in China had serious chronic hepatitis B liver infection, doubled with alcohol damage which led to a sudden deterioration in his liver function. In an effort to save his life without a donor organ available, he was connected to a pig liver outside his body — a procedure called extracorporeal perfusion – so the pig organ could filter the man’s blood while he was waiting for a human liver transplant. According to the Chinese surgeons who performed the procedure, the man has since received a human liver and is recovering well.
Pig organs are anatomically and functionally similar to human organs but obviously not identical. To reduce the risk of the recipient rejecting the organ, the pig liver contained six genetic modifications - three deactivating pig genes and three introducing human genes. The surgeons stitched tubes to a vein in the man’s leg, connecting him to a perfusion device containing the pig liver. His blood was redirected through the pig liver so it could remove harmful waste products just like any other healthy liver. According to his doctors, the patient showed no signs of organ rejection, and his own liver function began to improve. The man was disconnected from the perfusion system after three days to reduce the risk of infection and complications.
The procedure is a bridging therapy that allows a person’s organs to recover, or a patient to survive long enough to receive a lifesaving human donor organ. Extracorporeal perfusion using pig organs has been performed since the 1990s, but the development in recent years of genetically modified pig organs that are more compatible with humans have significantly reduced the risk of organ rejection. There is still a lot we don’t understand, but research is currently underway to understand the potential, limits, and optimal parameters of this procedure. Last year, the US Food and Drug Administration approved a trial to test whether extracorporeal perfusion using genetically modified pig livers can be used to safely treat people with organ failure. The trial is currently recruiting participants. The road is still long, but expert believe that one day, pig organ transplants could be superior to human ones.
Last edited: 7 April 2026 10:59