Organ transplants
What is organ transplantation?
Organ transplantation is a life-saving medical procedure involving the removal of a healthy organ from a donor and placing it into a patient with organ failure. First successfully performed in 1954 when a kidney was transplanted between identical twins, organ transplantation has since developed into a highly sophisticated field, benefiting patients suffering from terminal liver, heart, lung, kidney, and pancreatic diseases.
Advances in surgical techniques, immunosuppressive therapies, and post-operative care have improved patient outcomes and the viability of transplanted organs, offering hope for thousands who face life-threatening organ failure.
While the science of organ transplantation steadily advances, the global shortage of suitable human transplant organs remains a problem. In the UK alone there are around 7,500 people on the waiting list to receive a transplant organ. The scarcity of suitable transplant organs has spurred research into alternative solutions, including xenotransplantation, the use of animal organs, typically from pigs, for transplant into humans. Animal research plays a critical role in the development of safe transplantation practices and in studying immunological rejection, infection risks, and the viability of cross-species transplantation.
The first organ transplants in history
The first mention of transplant surgery dates back to 1,550 BC, found within the Ebers papyrus, a compilation of ancient Egyptian medical texts. The papyrus describes skin grafting for the treatment of severe burns, but it was a long journey from those early successes to the modern era of organ transplantation which begins in earnest in the late 1800s with the growing scientific drive to better understand the role of organs within the body.
Research in animals has been essential at every stage of that journey, to determine the function of organs, to test surgery methods, to solve the issue of organ rejection, and most recently as a potential source of organs for human recipients.
Investigating hypothyroidism with transplantation
Pioneering surgeon Theodor Kocher (1841–1917) began to notice an “unknown syndrome” in patients who had undergone a full thyroidectomy. This condition, later recognised as hypothyroidism and historically described as cachexia strumipriva, prompted efforts to understand the function of the thyroid gland. The quest to uncover the cause of this syndrome marked the beginning of decades of animal research into organ function and replacement. Thyroids and other organs were removed from animals in order to observe the effects on the body, with surgeons testing their conclusions by grafting or transplanting tissue to see whether symptoms could be alleviated.
In experiments using dogs and monkeys, Sir Victor Horsley demonstrated that removal of the thyroid caused severe neurological and systemic disturbances, and that transplantation of thyroid tissue could temporarily improve the condition. Similarly, the experimental removal of the pancreas in dogs by Oskar Minkowski and Joseph von Mering showed that diabetes develops when the pancreas is absent. Subsequent research established that this effect was due to the failure of the islets of Langerhans within the pancreas.
Together, these experiments helped lay the foundations for our modern understanding of the role played by different organs in the body and their relationship to disease.


Theodore Kocher © Association of Surgeons of India 2012 Victor Horsley © G.C. Beresford, via Wikimedia Commons
Organ transplants in dogs
The first heart transplant was carried out in a dog in 1905, by Carrel and Guthrie. They removed a dog’s heart and transplanted it heterotopically (alongside the existing organ) into the neck of a recipient dog. The heart began beating one hour after the surgery and continued to beat for two hours before coagulation occurred. Dr Alexis Carrel was awarded the Nobel Prize in 1912 for this and other work on heart transplants.
Further experimental transplants in dogs were carried out by other researchers, including the first liver transplant in 1955 by Dr. Stewart Welch, whose work helped lead the way to the first liver transplant in humans in 1967.
Fixing the organ rejection problem
For many years organ transplantation was confounded by the problem of rejection. Unless the donor and the recipient were twins, and therefore genetically identical, the immune system would identify the donated organ as alien and treat it as a threat. In 1962, Dr. Roy Calne and his team at Peter Bent Brigham Hospital, published findings that 6-mercaptopurine, an immunosuppressant drug, prolonged survival after kidney transplant in 104 dogs. This led to further studies in humans, where three immunosuppressant drugs were determined to be effective at reducing organ rejection between genetically diverse patients. For the first time, organs could be transplanted between people who were not genetically related.
Organ donation from deceased donors
Much early research into transplantation focused on kidneys because they were the only organ that could be transplanted without causing harm to a living donor. For transplantation to be an effective therapy for diseases in other organs, it was essential that scientists found a way to use organs from deceased patients. After carrying out more than 400 lung transplants on dogs, Dr. James Hardy and his team at the University of Mississippi, were able to transplant the first human lung from a deceased donor in 1963, marking a huge milestone in the field.
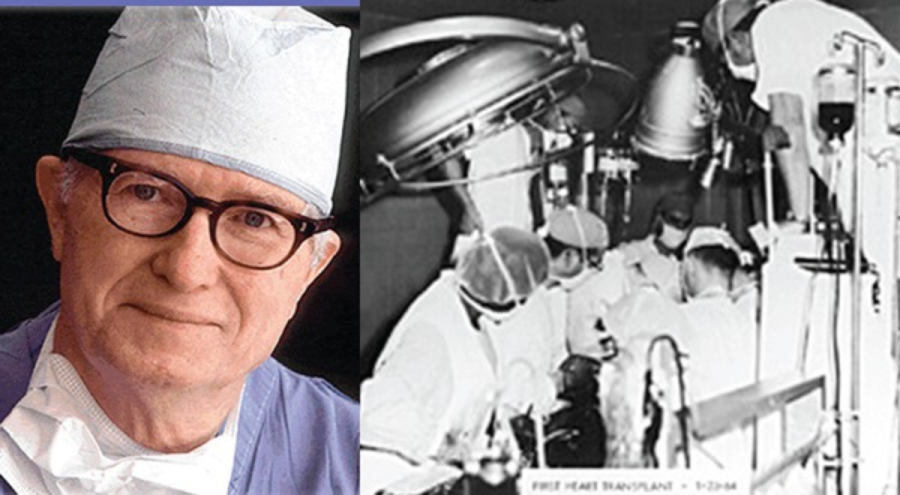
On the left, Dr. James Hardy, on the right, a photograph of the operating room of the first human xenotransplantation.
© Braz J Cardiovasc Surg. 2017 Sep-Oct;32(5):423–427. doi: 10.21470/1678-9741-2017-0508
Animal research into xenotransplantation
Xenotransplantation is the transplantation of organs between different species and is considered one of the most promising solutions to the shortage of available organs for transplant.
Early xenotransplantation attempts were not successful. Failures included the attempted transplant of a rabbit kidney into a child in 1905, and a lamb kidney into a human in 1923. Both of these cases resulted in patient death or transplant failure within days.
Between November 1963 and February 1964, Keith Reemtsma carried out the first successful xenotransplants. At the time, few human organs were available, and dialysis was not yet available as a treatment for kidney failure. Thirteen patients received chimpanzee kidneys, with survival ranging between 11 days and two months, except for one patient, who returned to work for nearly nine months before dying suddenly. Despite the short survival time, the outcomes were considered an overall success by the transplant community.
Liver transplants from monkeys to humans were also attempted in the 1960s, although the results were not considered successful enough to warrant human clinical trials.
For many years after that xenotransplants were attempted but no long-term results were achieved due to the biological differences between humans and donor animals. Things only began to change in the 21st century. With the advent of CRISPR/Cas gene editing tools, pig organs could be genetically modified to be more compatible with the human body, making xenotransplants a realistic proposition in the near future with some success already achieved.

Keith Reemtsma (1925–2000). © Int J Surg. 2015 Jun 26;23(0 0):205–210. doi: 10.1016/j.ijsu.2015.06.060
The first pig-to-human heart transplant
In January 2022, David Bennett, a 57-year-old man with terminal heart disease, became the first person to receive a pig heart transplant. This life-saving procedure was performed at the University of Maryland Medical Center after Bennett was deemed ineligible for a human heart transplant due to his poor health. The pig's heart had undergone extensive genetic modifications to reduce the risk of rejection, including the inactivation of genes that trigger immune responses and uncontrolled growth. Bennett survived for two months post-surgery, highlighting both the potential of xenotransplantation and its challenges, such as immune rejection and pathogen transmission. This pioneering effort represents a significant milestone in medical science, offering hope for reducing transplant waiting times and saving lives in the future.
Pig kidney transplanted into a living person
In March 2024, a groundbreaking procedure was performed at Massachusetts General Hospital, where a genetically modified pig kidney was successfully transplanted into a living human recipient, marking a significant milestone in xenotransplantation. This achievement followed years of research into genetic modifications that reduce rejection risks, such as the knockout of the alpha-gal antigen, which has been crucial in preventing immune system rejection. Despite initial successes, challenges remain, including the need for long-term anti-rejection medications and addressing potential blood coagulation issues. While early results from compassionate use cases have shown mixed outcomes, with some recipients experiencing complications, researchers remain optimistic about the potential of pig kidneys to alleviate the organ shortage crisis.
The longest person to survive with a pig organ
In 2025, Tim Andrews, a 67-year-old man from the USA, was implanted with a genetically modified pig kidney. At first, the kidney appeared to be functioning well and Andrews no longer required dialysis treatment. Unfortunately, after nine months, it became clear that the genetic modification of the donor pig, and the addition of immunosuppressive drugs, was not enough to prevent organ rejection. While the kidney was ultimately removed, Tim Andrews lived with the gene-edited pig organ for a record-setting 271 days, marking a significant milestone for the field of xenotransplantation, and the longest any person has lived with an organ transplanted from an animal.
Tim Andrews, the longest person to survive with a pig organ © Massachusetts General Hospital: Kate Flock
Xenotransplant techniques available for treatment
There are some xenotransplant techniques which have succeeded in human clinical trials. in 2016, Chinese regulators approved the use of pig corneas to restore the sight of 200 patients with corneal disease. That same year, surgeons safely transplanted pig pancreatic insulin-producing cells into humans without the need for immunosuppressive drugs after they had cured diabetes in five baboons.
The future of animal-to-human organ transplants
Given the high rate of failure in the early days of human-to-human transplant research, it is no surprise that animal-to-human transplants are still a long way from being standard practice. The clinical research is in its early days, with only a handful of people having undergone xenotransplantation. Many of these procedures did not result in long-term success but have given valuable insights on how to improve the procedure in the future.
While there has been great success in transplanting smaller organs, such as pig corneas and pancreatic insulin producing cells, it is clear that more research is required to perfect xenotransplantation for larger organs such as the heart, lungs, and kidneys. Scientists are particularly focused on refining genetic engineering for donor pigs and limiting the potential risks from the use of CRISPR/Cas gene editing techniques. Other avenues such as the possibility of growing human organs within genetically modified animals are also being explored and more research will be needed to better understand the possibly unknown and difficult-to-detect animal pathogens that might pose a risk to humans.






