 Although nearly 85% of Nobel Prizes in Physiology or Medicine have relied upon animal research, a few laureates have used themselves as guinea pigs. Below, UAR details some of these self-experimenters, who each took a risky step for their own reasons – bravery, desperation and hope.
Although nearly 85% of Nobel Prizes in Physiology or Medicine have relied upon animal research, a few laureates have used themselves as guinea pigs. Below, UAR details some of these self-experimenters, who each took a risky step for their own reasons – bravery, desperation and hope.
Werner Forssmann – Winner 1956
In the 23 years preceding winning the Nobel Prize, Werner Forssmann had worked as a urologist, served as a Major in the German Army and was captured as a prisoner of war. But none of that concerned the Nobel committee, who were honouring Forssmann for his work as a young surgical intern when he first demonstrated cardiac catheterization in a human: himself.
Generally thought to be impossible without causing severe damage to the heart, cardiac catheters require inserting a catheter into a vein and threading it through until it reaches the heart. This would allow clinicians to measure the pressure in the heart and determine if a defect needs to be operated on. Inspired by researchers who had achieved this in a horse in 1861, Forssmann saw the potential this technique could have.
Refused permission to experiment on patients, Forssmann set out to test the technique on himself. First he had to convince the operating room nurse to give him access to surgical instruments. She relented on the condition that Forssmann would place the catheter in her instead, which he accepted. However, once he had strapped the nurse down onto the operating table, Forssmann quickly anaesthetised his own arm, made an incision and inserted the catheter 30 cm along his veins. He then walked up two flights of stairs to the x-ray room before extending the catheter the full 60 cm to enter his heart and taking the picture shown above.
Forssmann’s reckless bravery generated much annoyance and excitement. The annoyance eventually won out and Forssmann was forced to withdraw from his residency. Although he moved out of research, Forssmann’s paper on his work was read many years later by André Frédéric Cournand and Dickinson W. Richards who built on the technique and shared the Nobel Prize with him. On hearing news of the Prize, Forssmann said, ‘I feel like a village parson who has just learned that he has been made bishop.’
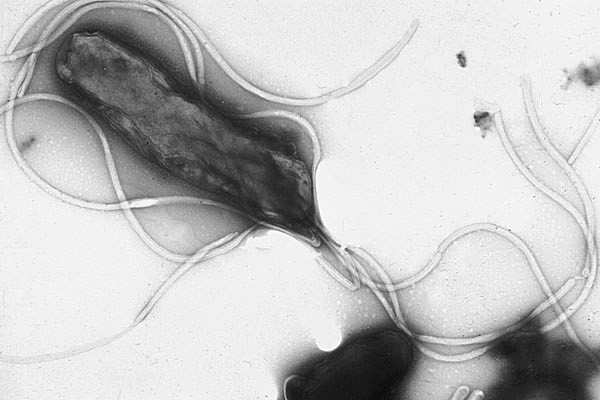
Barry Marshall must be the poster boy for self-experimenters everywhere. He drank a heady broth of bacteria from the lab to prove to his peers that the bacterium Helicobacter pylori was the cause of stomach ulcers.
Stomach ulcers were long thought to be due to stress, with the only treatments being rest, anti-acids, and surgery in extreme cases. But in 1979, pathologist Robin Warren noticed inflammation in regions of stomach biopsies that were colonised by small, curved bacteria. Marshall, intrigued by his findings, contacted Warren and the pair began a survey of 100 patients and biopsies. For them, it became clear that the bacteria, which they named Helicobacter pylori, were the cause of stomach ulcers and gastritis.
This discovery was a radical departure from medical opinion at the time, and many researchers and doctors were sceptical. The presence of the bacteria and inflammation did not prove cause and effect. With no suitable animal model susceptible to the bacteria (this was before the Mongolian gerbil had been found to model the human condition), Marshall decided to demonstrate the role of bacteria using himself as a guinea pig.
Five days after drinking the broth, he began to experience loss of appetite before then vomiting regularly each morning. An endoscopy revealed the truth: Marshall had given himself gastritis. Under orders from his wife, Marshall began taking antibiotics and the symptoms subsided. This proved that peptic ulcers and gastritis could be cured, saved thousands of lives and rendered the billion-dollar industry of previous treatments obsolete.
When Ralph Steinman was announced as one of the winners of the Nobel Prize in 2011 friends, colleagues and journalists were quick to try to contact him. Outside of his family, no-one knew that he had died just three days earlier.
Along with Bruce Beutler and Jules Hoffmann, Steinman was being honoured for his work on the immune system. He had discovered a new type of cell, which he named dendritic cells because of their tree-like structure, that activate T-cells to fight off an infection. The immune system is primed to attack foreign and unusual cells in the body, but some cancer cells can slip past its defences. Being able to control the dendritic cells would allow researchers to train them to target camouflaged cancer cells.
This was a new approach, highly experimental and likely to take decades before it could be available to the public. So when Steinman was diagnosed with advanced pancreatic cancer in 2007, he saw the opportunity to start a human trial and potentially buy himself more time. He had little to lose, with less than a five per cent chance of surviving a year. Dozens of his colleagues and collaborators came forward with ideas and techniques for improving his ‘experiment’. They worked to grow portions of the tumour in mice, test the effects of different drugs, sequence the cancer’s DNA and extracted proteins from the surface of the cells. In addition, Steinman received three different, personalised vaccines that were based on his work on dendritic cells. Steinman received eight experimental treatments, in addition to conventional chemotherapy.
Despite the range of these treatments, Steinman still succumbed to the cancer but he had survived four and a half years – far longer than expected. Although he never learned that he had won the Nobel Prize, he was sure that his work had prolonged his own life and may one day extend many more.
Last edited: 11 March 2022 08:53