Multiple sclerosis (MS) is the most widespread disabling neurological condition of young adults, particularly women, around the world with around 2.3 million people living with MS globally. In MS, the protective insulating myelin sheaths that cover nerve fibres in the brain and the spinal cord are destroyed.
This damage disrupts the ability of parts of the nervous system to communicate which causes a wide range of physical, mental and sometimes psychiatric symptoms. While the cause of this disease isn’t clear, it is thought to be linked either to the destruction of the myelin sheaths by the immune system or to a failure of the myelin-producing cells.
To this day, there is still no known cure for MS. Treatments attempt to improve lost function and prevent further damage but they are not very effective and can have side effects. In order to treat the disease properly, it is important to understand it.
Dr Anna Williams from the Centre of Regenerative Medicine in Manchester is particularly interested in trying to understand how the brains of patients with MS repair. Indeed, the brain has the possibility to put myelin sheaths back onto nerves, which has the potential to restore nerve function in MS. However, this process is generally inefficient, and often forms scars which can cause long-term problems for patients. Cells that have this repair function are called oligodendrocytes. The research team has looked into how these cells work and whether they could get them to repair myelin damage more effectively.
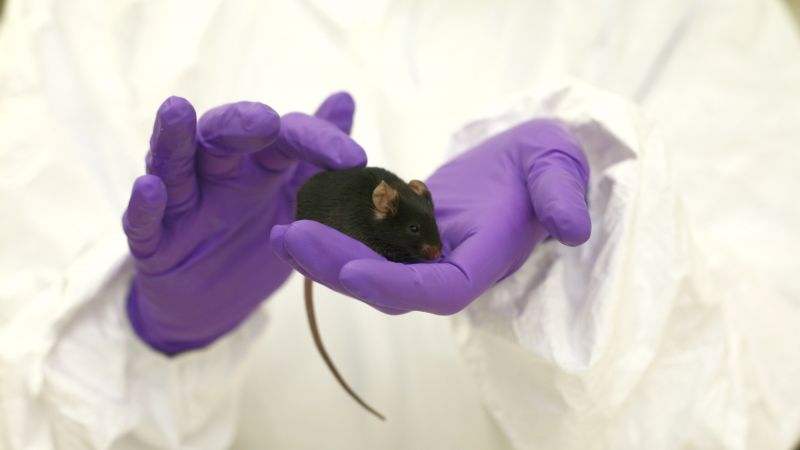
By growing oligodendrocytes in dishes, it is possible to monitor whether they make more or less myelin depending on different conditions or drugs. The team does a lot of experiments using cells from mice, rats and humans and slices of brain from mice and rats.
“Ultimately, the work moved to live animals. As humans are the only animals that get MS naturally, we therefore tried to model part of the disease in mice. We’re interested in myelin repair, so we caused a small amount of demyelination in the animals by chemical-injection in the brain. The mice don’t seem to be affected by this. Mice repair their brains much better than humans do. So within 4 weeks, basically all signs that myelin damage goes away,” explains Dr Anna Williams.
“The mice don’t develop symptoms but imaging of the brains can give us a before/after treatment picture to see how well oligodendrocytes are repairing myelin. We measure the pathology rather than the pain.”
There are currently three drugs that have entered human trials for trying to improve myelin repair in MS after studies in animals. Dr Anna Williams worked on one of them called Baroxatine.
“About 10 years ago we started to look for a drug that could help oligodendrocytes make more myelin. After finding positive results in cells, brain slices and animal experiments, we moved to a clinical trial in patients. That trial has now finished but the results aren’t available yet – they are being analysed as we speak.”
In the meantime, Dr Anna Williams has recently showed that human oligodendrocytes obtained from post-mortem human brains are different from the ones in mice or rats. And although that might sound like bad news, the fundamental differences between the species might actually be a clue to finding a cure for MS.
“Comparing human cells and mice cells might give us an answer as to why human brains don’t repair as well as mice brains, and how to improve them. Building on this finding, we could also improve our current animal models by using genetics to make mice cells more like human cells or integrating human cells into our mouse models,” concludes Anna Williams.
Image: https://en.wikipedia.org/wiki/Oligodendrocyte#/media/File:Oligodendrocyte.png
Last edited: 4 March 2022 09:16