Chris Magee considers the use of animals' reactions to drugs to gauge the probability of human harm, with data from an unexpected source.
Of the many, various, manifold misconceptions manufactured by anti-research activists, one of the toughest nuts to crack is that of animals being ineffective models for human toxicity. This claim is made up of simple parts, exploiting popular misconceptions about what research is, including the idea that all or most of research is using animals to test pharmaceutical safety and presenting interspecies differences as an impossible scenario rather than one consideration in your choice of model.
So the narrative goes, differences between species mean that they all react differently to drugs so animals cannot predict human reactions!
This will usually be accompanied by a genuine example where one species really is a rotten model for a particular type of drug or condition and sometimes with a nod to genetic differences, because did you know just a small genetic variance can have a big impact on physiology?!
To be clear, interspecies difference is a thing, but a thing that is generally accounted for by choosing the right species for your study. In the hands of activists, however, it becomes some sort of insurmountable barrier to any animal models ever working.
Riding in the sidecar of this horrendous misrepresentation of interspecies difference is usually one of the handful of examples of clinical trials gone wrong dropped in as if it’s one of a long list rather than the only serious incident in the UK in 30 years and/or mutterings about ‘side effects’, as if these aren’t literally listed in a booklet that comes with your medicines.
It’s a difficult one to counter for a number of reasons, not least the sheer number of not-quite-on-the-money misconceptions underlying activists’ understanding of how research is conducted and the fact that animal toxicological data - that would quickly settle the argument - is often hiding in pharma companies’ confidential files or behind toxicology journals’ paywalls.
At least it was a difficult one to counter. In 2013 and 2014 excellent data from an improbable source - anti-research campaigners – gave us a great, publicly available, insight into what toxicologists knew all along: the right animal models mimic toxic human reactions.
Before we get to the data, though, let’s be clear about what we mean by ‘predict’. Most animal research isn’t trying to predict anything. The use of the word by activists is itself an attempt to constrain any debate and force it away from Nobel Prize-winning basic research and onto the niche territory of tox testing where they think they can ‘win’.
One might say, correctly, that people can react differently to drugs, therefore how can someone predict what will happen if you take a given compound? Well, they can’t really but then they’re not trying to. Unless they test your DNA, which doctors would still do only rarely, they wouldn’t spot something like a genetic resistance to blood thinner Plavix if you visit A&E but might infer it from your reaction to the standard dose, and increase the dose (the Plavix doesn’t become useless in the face of genetic resistance, which is the implication of activists).
No, the sort of ‘prediction’ we’d be talking about is more a probability. About 25% of humans are somewhat resistant to Plavix, which means that 75% aren’t. The standard dose, unsurprisingly, is tailored to the 75% not the 25% because you personally are probably not resistant to it, but doctors are well accustomed to fiddling with dosages until efficacy is achieved for the individual patient – it’s not some sort of revelation that drugs work slightly differently in different people. It’s the same with all medication from blood pressure drugs to insulin.
Even your genetic predispositions won’t allow complete personalisation of your drugs because of differences in absorption, body weight, metabolism etc that are implied but not mandated by certain genes. The claim for drug efficacy is simply ‘this drug can help lower blood pressure’ or ‘this drug can lower blood sugar’. It doesn’t claim to know by how much in each individual in each situation, which is why hospitals have consultants to help people personalise their treatment.
Similarly, I could say to you that smoking may give you cancer, and I could calculate both the increased risk and maybe your personal probability if I knew enough about you, but the fact I couldn’t say for sure it would definitely, definitely happen doesn’t make it any safer to do.
It’s really this sort of thing that we’re talking about when it comes to medical research. Making ‘prediction’ a completely precise form of precognition is one of the standard pillars of science denial – setting the bar of proof impossibly high, like claiming climate change is nonsense if a climate scientist can’t predict tomorrow’s weather.
So, how can animals be used in pharmacology tox testing and how effective are they as indicators of human reactions?
Well, firstly let’s be clear what they’re being used for. Before drugs go onto human trials (‘clinical trials’) a battery of tests are used to try to see if the proposed dose is likely to hurt a human volunteer. These include all manner of models – computer models, animal models, cell cultures – the ‘alternatives’ to animals that are often spoken about are already in use alongside animal models.
A candidate compound is tested on animals, using one rodent and one non-rodent species. Each has its own probability of inferring a positive or negative human response, but combining species data has been the norm for many years because if something’s toxic in both a rodent and a non-rodent it’s odds-on toxic to humans. As an aside, the NC3Rs and pharmaceutical body ABPI are currently running an investigation into how much extra confidence that second species really provides now that we’ve gotten better at deriving the right answer from just one species.
So what sort of probabilities are we talking about?
Well, generally over 90%, but as I mentioned this answer comes from an unexpected source.
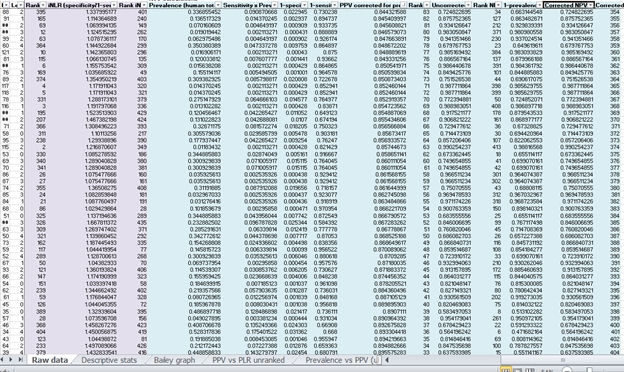
In 2012, the Chief Executive of the British Union for the Abolition of Vivisection (BUAV), one of her employees and the Chair of the Fund to Replace Animals in Medical Experiments (FRAME), Michael Balls, assembled an exceptional data set covering 2,366 drugs for which there was human and animal data available from FAERS, the FDA and DrugBank. Their aim was clearly to prove once and for all, in a scientifically robust way, that animals didn’t predict human tox reactions. Obviously, this data set is slightly skewed because we wouldn’t have given a drug that harmed a test animal to a human just to test the theory, but it’s as good as it’s possible to get.
Now, I wasn’t in the room but I think I can see how this went down. I think they took the data set, I think they ran it through Bayes’ Theorem (statistical modelling which gives us true positive and true negative predictive values), I think they saw the numbers you’re about to see, I think they went ‘oh dear’, and I think they went casting about for a statistical model that better fit their existing worldview that the experiments were not worthwhile. They then put that in a paper in a journal that is edited by one of the paper's authors packing an impact factor of 1.021 where, if it was peer reviewed, the peer reviewer failed to notice the authors’ serious errors such as failing to analyse half their own data.
Meanwhile, the rest of the world uses Bayes' theorem to find positive and negative predictive values (PPV and NPV respectively) which are the proportions of positive and negative results in statistics and diagnostic tests that are true positive and true negative results, not false positives/negatives. The PPV and NPV describe the performance of a diagnostic test or other statistical measure.
Over 4 species, the PPV and NPV were thus:
|
|
PPV |
NPV |
|
Dog |
70% |
94% |
|
Mouse |
92.9% |
95.6% |
|
Rat |
90.5% |
97.9% |
|
Rabbit |
98.8% |
99.2% |
Oh, boy. We haven’t even combined species data yet, or applied various other tricks to push these numbers higher.
So, what genuine scientists would do at this point is say ‘huh, guess I was wrong’ and change their view (if their view was animals don’t predict human responses). Indeed, after sitting in the crowd of the 2013 FRAME lecture, where the data was unveiled, I approached co-author Dr Bailey to say exactly this – that if this data checked out and supported their idea that animals don’t predict human reactions we’d happily back any calls for change.
“If”.
Of course, we got the data home and saw what they’d done instead of changing their minds, which was use a perfectly fine alternative statistical model which showed a weaker correlation between human and animal responses to analyse the data, but try to argue unconvincingly that this model should displace Bayesian modelling which gives us the numbers above.
The bare numbers derived from the Bayesian interpretation not only provide an easy-to-see impression about the efficacy of animal models in this area, but also make the attempts of activists to flesh out their ‘interspecies difference’ meme with science-y sounding reasoning (Ray Greek), scaremongering over ‘side effects’ (Safer Medicines Trust) and false equivocations about each species needing unique medicines (Andre Menache) look a bit silly even to the layperson.
They become someone standing at an airport arguing at length - using graphs and formulae, and tales of twisted metal and claims that man cannot travel above 40mph - that airplanes cannot fly.
Of course, the similar reactions of many, not all, species to various drugs is what lies behind the One Health initiative where, for instance, human drugs might be adapted for veterinary use – which is usually just a matter of dosage. It wouldn’t work if humans and other animals were irreconcilably different in all ways from one another, and the fact that it’s being used to great effect right now by veterinarians is a great deal more compelling than a theoretical reason why it mightn’t work.
For completeness, it’s worth dredging up interspecies difference’s partner in crime “92% of drugs that pass animal tests fail in humans” which is a tricksy and misleading statement we’ve looked at before. In essence, it doesn’t refer to just animal models, but all models used before human trials – computers, cell cultures, organs on chips and refers to safety testing, wherein a drug may ‘fail’ because it’s safe but not effective, or not marketable, or not the first to market, or any other reason that would make it worthwhile discontinuing that avenue of research. Indeed, by the same metric, 86% of drugs that pass stage 1 human trials, which test for safety, ‘fail’ by stage 3 – but not because they’re acutely dangerous or the animal data were misleading.
The leading founder of the anti-vivisection movement, Frances Power-Cobbe, didn’t get everything right, but might have been onto something when she warned activists 120 years ago not to try to denigrate the science or efficacy of animal research. As she put it:
“We have gone on off our rightful ground of the simple moral issues of the question (and have seemed to admit what very few of us would deliberately do), that if some important discovery had been made by vivisection, our case against it would be lost or weakened. I have been so anxious to warn our friends against this, as I think, very grave mistake on tactics...”
As ever, the real casualties here are those genuine potential issues with animal research (such as the poor experimental design which haunts all areas of science or failure to observe the animal-specific ARRIVE guidelines) which get sidelined when activists make bombastic claims. This only elicits a bombastic response that must spend its time unpicking the misconceptions about how research is undertaken to get everybody back to zero, rather than anyone advancing a nuanced view of what could be better – the only approach, in fact, which will ever effect the change activists and scientists alike would want to see.
I would certainly rather be in a different space, and activists presumably want to make more progress than the startlingly little they’ve managed these past 150 years by making stuff up.
Last edited: 29 July 2022 14:25

