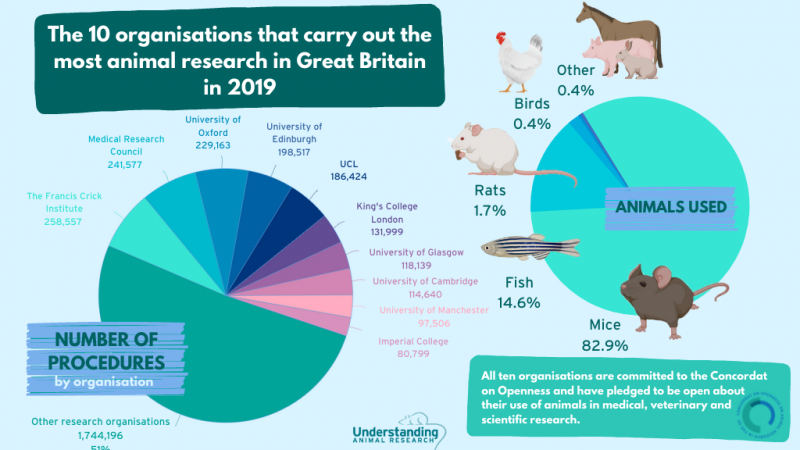
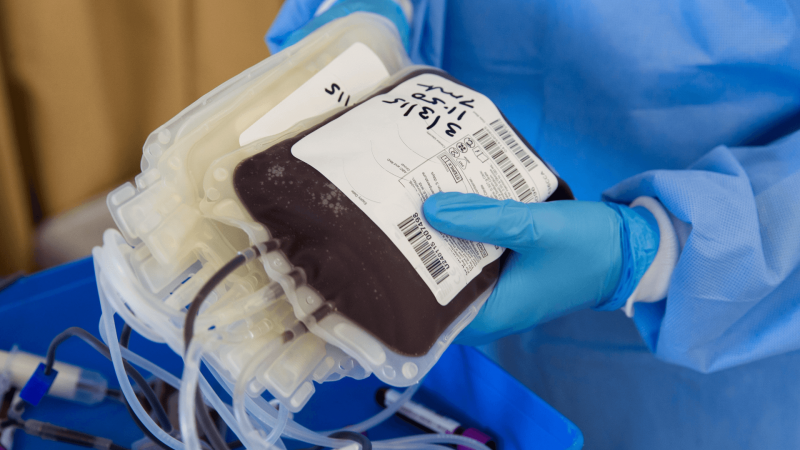
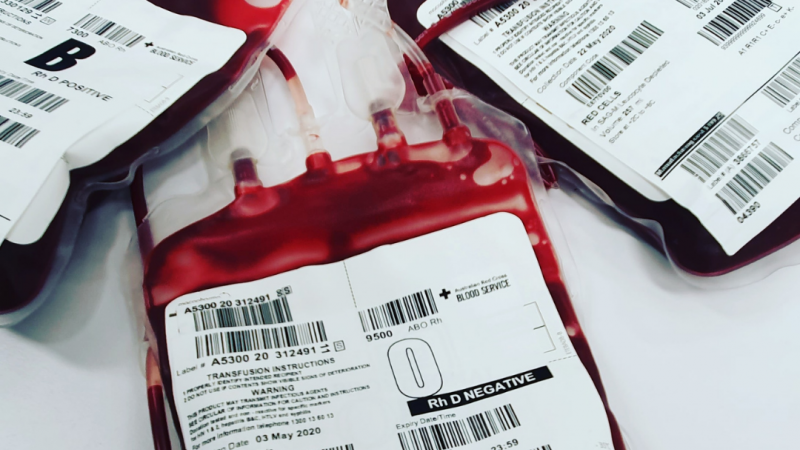
Every year, over 88 million blood donations save lives across the globe – enough to fill 32 Olympic-sized swimming pools with the haemoglobin-rich liquid. But good quality blood is in short supply so researchers seek to get around the worldwide blood shortage and make blood donations as we know them obsolete.
Animal research has been instrumental in conceiving, optimising and now upgrading this life saving procedure.
Transfusion dates back more than 300 years, when in 1657 the anatomist, astronomer, architect, and mathematician-physicist Christopher Wren, famous for the design of Saint Paul's Cathedral in London, claimed to be able to create a tool that would allow him to « convey any liquid poison into the mass of the blood ». He used a syringe made of animal bladder fixed to a goose quill to inject wine and opium into the veins of a dog.
The technique was later refined by British physician Richard Lower who performed the first-ever successful animal blood transfusion in 1665 on a dog.The first-ever animal to human transfusion of blood was performed closely after, in 1667 by Frenchman Jean-Baptiste Denis who transferred blood from a sheep to a 15-year old boy and a woman in labour. Both survived the process but with severe anaemia, throwing a black cloud over the technique.
For a long time, blood transfusions remained a technically difficult procedure . Even when Karl Landsteiner defined the blood types in 1900, and recipients and donors could be precisely matched, transfusions were rarely attempted. It was Adolph Hustin that made in 1914 the discovery that would tip the boat in favour of the lifesaving technique. He found that adding sodium citrate to the blood prevented it from clotting and allowed it to be stored safely for several days. Years of animal research in dogs, rabbits and guinea-pigs to perfect transfusion coupled with the capacity to store blood led to blood banks and blood transfusions to become the routine procedure it is today.
But nowadays, the human population is confronted with a shortage of blood to transfuse and researchers are turning back to animal research to find solutions to this critical health problem and make blood donations, as we know them, obsolete. In 2011, for example, a blood substitute derived from cow plasma was used to save the life of a woman whose religion forbade conventional blood transfusion. This artificial blood is designed to increase oxygen transport in the body after heavy blood loss.
Some animals can transport oxygen more effectively in their body than humans. The marine lugworm, Arenicola marina is a champion oxygen-hugger. Indeed, the worms breathe through gills, like fish, but they spend half their lives out of water where they can survive for 6 hours without breathing. This is possible thanks to their special haemoglobin, the proteins in blood that carry oxygen, that is 40 times more oxygenating than its human counterpart. In human blood, one haemoglobin protein holds four oxygen molecules at a time whereas a lugworm haemoglobin protein can hold an amazing 156 O2 molecules, according to the researcher Franck Zal. And the more he looked into these worms, the more special the worms’ blood became.
As it turns out, the lugworm is a universal donor – it doesn’t carry any antigens on its surface that are responsible for the different blood types. This means that it can be used in humans and could change the face of medicine. In 2016, the first clinical trials tested the efficacy of the worm blood and showed that transplant organs stored in Hemo2Life worm blood allowed for a faster patient recovery and improved organ function compared to transplant organs stored in the traditional electrolyte preservation solution. In fact, the lugworm’s haemoglobin is so effective at transporting oxygen that organs immersed in their solution can survive for days without damage, rather than hours.
Since those tests, Hemo2Life has been used to safeguard a variety of organs, including lungs, pancreases, and a heart. It was even used in 2018 in France, for the first ever second full face transplant and was instrumental in the procedure according to the surgeon, Pr Lantieri who stated “I will never do another transplant surgery without this product “.
Franck Zal’s company, Hemarina, is in the process of applying for certification to sell Hemo2Life throughout Europe and could provide enough Hemo2Life for all the organ transplants in France and still have more than one tonne of worm blood left over.
Zal has set his sights on other uses for lugworm blood such as worm blood bandages to treat chronic wounds, or a haemoglobin-based oxygen carrier that could be used to treat sickle cell anaemia and even a gel-like oxygen carrier as a promising therapeutic solution for the treatment of periodontitis.
Last edited: 7 April 2022 13:31